Navigating Shoulder Surgery: What to Expect Before, During, and After
Shoulder surgery can sound stressful, especially after an injury. You may feel pain every day. Simple tasks like lifting your arm or even sleeping become hard. So, what happens when rest and therapy don’t work anymore? Surgery may be the next step.
Knowing what to expect helps you feel more ready. Got into a car crash, slip & fall, or suffer from other personal injuries? Then, this guide is for you.
You’ll learn what happens before, during, and after shoulder surgery. This includes tests, how the procedure works, and what recovery might look like. Many people also want to know how long healing takes or how they’ll sleep after surgery. We’ll walk you through all of it.
At Surgery Consultants of Florida, we help patients who are injured in car crashes, falls, or other accidents. We offer surgeries and care plans tailored to your injury.
We’re here to support you through every step of the process.
What Happens Before Shoulder Surgery: 5 Key Things You’ll Go Through

Getting ready for shoulder surgery can feel overwhelming. But knowing what’s coming helps you stay prepared.
These steps are important for your safety and better results. Here’s what you can expect before the procedure.
Medical Checks and Imaging Tests
Your doctor will look at your medical history. You may need blood tests or scans like X-rays or MRIs. These help your care team learn more about your injury and check your overall health.
Changes in Medication Use
Some medicines can affect healing or cause bleeding. You might need to stop blood thinners like aspirin. You could also be told to pause herbal products like garlic pills. Always follow your doctor’s list and ask if unsure.
Talking About Anesthesia Options
You’ll meet with the anesthesia team. They’ll go over different choices like full sleep or a numbed arm. Your body condition and comfort will help guide the final plan.
Shoulder Area Prep and Marking
Right before surgery, the team will mark the incision sites. This helps lower the risk of nerve or blood vessel injury. It also helps with better results and healing.
Getting Your Home and Schedule Ready
You’ll need a setup for rest at home. Stock up on food and easy-to-reach supplies. Make sure someone can drive you home. Time off work may be needed depending on your recovery.
What Happens During Shoulder Surgery: 5 Key Steps You Should Know
Going through shoulder surgery can create worry. Clear details help ease that stress. You will feel more ready once you know what happens in the operating room.
Knowing what to expect can also guide safer care and smoother shoulder surgery recovery.
Care Team Setup Before Repair
Staff place you on a padded table. Your shoulder area gets cleaned with care. Devices check heart rhythm and oxygen during your procedure.
Anesthesia Given for Comfort
An anesthesia plan keeps you pain free. You either stay asleep or your arm stays numb, depending on your plan. Staff watch your comfort closely.
Small Cuts for Camera Access
Your surgeon makes tiny cuts for tools. A small camera enters through one cut. Larger cuts happen only when needed for better access.
Repair Work Based on Injury Type
Damage guides each repair method. Surgeons fix torn tissue or reattach tendons when required. Many cases use less invasive steps to achieve quicker healing.
Closing Cuts With Careful Technique
Sutures or glue close each cut securely. A clean dressing goes over your shoulder for protection. A sling may support your arm after surgery.
What Comes After Shoulder Surgery: 5 Things You Should Be Ready For
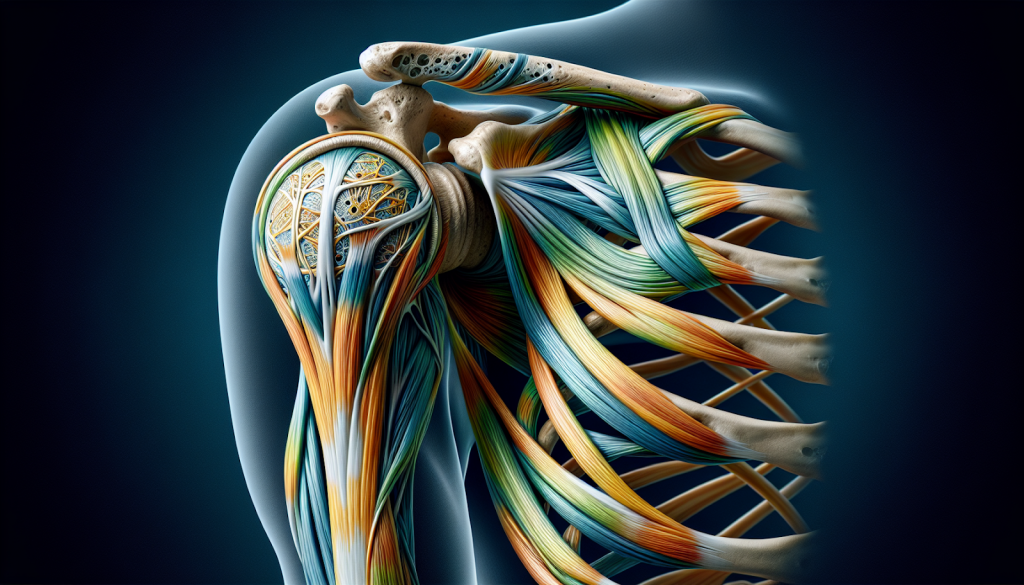
Understanding what to expect after shoulder surgery can help you stay on track. Your recovery may feel slow at first. That’s normal.
Each day brings small progress. Here are five important things you’ll go through once the procedure ends.
Expect Some Pain, But It Gets Managed
You may feel shoulder pain after surgery during the first few days. Doctors may give medicine for relief. Ice packs can help lower swelling. Resting your arm on a pillow may also bring comfort.
Wearing a Sling for Support
Your arm may stay in a sling or brace for weeks. This keeps the shoulder in place while healing starts. Try not to remove it unless your doctor says so.
Starting Rehab and Therapy Slowly
Physical therapy begins with light movements. It may feel hard at first. Over time, exercises help you regain strength. These early steps matter for full motion. This is why it’s important to follow your therapist’s guide closely.
Limits on Activity in Early Recovery
You’ll need time off from lifting and driving. Movements like reaching or pulling can cause damage. Follow your doctor’s rules as you return to normal tasks. Don’t rush this part.
Daily Care and Helpful Tips for Healing
Keep wounds dry and watch for signs of infection. Eat healthy foods with good protein. Stay on schedule with appointments. One of the best shoulder surgery recovery tips is patience.
Remember, healing takes time. Ask your doctor about how to sleep after shoulder surgery too. You may need to sleep upright with support pillows during the first few nights.
Need a Team You Can Trust for Shoulder Surgery? We’re Here for You
Getting shoulder surgery after an accident can feel like a big step. It’ll be a big help to have a team who’ll be there with you from start to finish.
You need support before, during, and after the procedure. The right care can make a big difference in your healing and recovery.
Experts in Injury-Related Shoulder Surgery
At Surgery Consultants of Florida, we focus on patients who have been injured in car accidents, have slip and fall cases, or suffered work-related injuries. Our team treats trauma-related injuries with care.
We’ve spent over 30 years helping people recover from serious shoulder damage.
Services That Focus on Your Full Recovery
Our care starts with a clear diagnosis, supported by imaging and tests. We create surgical plans that match your injury and lifestyle.
We handle procedures like rotator cuff repair, labral tear repair, and shoulder replacement. Our modern tools and skilled surgeons make sure you receive the right treatment.
Support That Goes Beyond Surgery Day
We don’t stop once the procedure ends. Our team also supports pain management, therapy planning, and rehab coordination.
You won’t go through recovery alone. Everything from surgery details to records is managed clearly and with care.
If you think shoulder surgery might be part of your recovery, contact us today.
Surgery Consultants of Florida is always here — ready to help you heal.